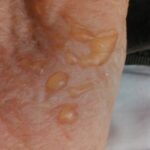
I received a call from a nursing home staff nurse who stated that this patient “suddenly had blisters appear on the right forearm, wrist to elbow. Every now and then you get a patient who is a poor historian and getting a past medical history is impossible. What do you do if you have a patient with little or no past medical history or you have a dementia patient with no family? Well, you need to become a great detective and make sure you do a thorough workup using a “Sherlockian approach”. Don’t trust 100% what is being told to you second hand, it can derail you. Make your assessment and gather your data with a thorough workup.
What we know is that the patient is male and 86 years old. The facility denies any changes in medications or environment. The patient has a history of dementia and no past history of bullae. At this time, a biopsy cannot be performed. The bullae are rupturing spontaneously and the nursing staff denies that the patient is in pain or noting paresthesia in that arm. No history of liver disease and patient is wheelchair bound and has not been outside (as far as they know). No known history of sensitivity to sun exposure or erythema/edema commonly seen with cutaneous porphyria.
Assessment: Multiple bullae right forearm with no erythema or edema noted. They are flaccid and break easily. No other vesicles or bullae noted on head, trunk or lower extremities. No other dermatoses noted.
Differentials (In order of suspicion): Bullous pemphigoid, bullous impetigo, drug eruption, contact/irritant dermatitis, epidermolysis bullosa, herpes infection, and porphyria.
Workup
Labs: CBC with diff, complete metabolic panel with LFT, ANA, U/A, Immunoglobulin panel, porphorin level, sed rate, HSV Panel and pemphigoid panel.
Cultures: C/S bacterial and viral
Treatment: Valtrex 1gm BID, Prednisone 40 mg PO tapered dose, Gentamicin ointment to open bullae QD and cover with non-stick dressing. Consider Doxycycline 100 mg BID x 10 days pending culture results.
Discussion: If herpes infection is suspected, I always wait to start prednisone after at least two doses of Valtrex are given. If there is any chance it is herpes virus, it is important to treat within 72 hours of vesicles/bullae. Delivery of medications are often unreliable and you should not give prednisone unless the patient has started the antivirals. If there is a chance of herpes zoster, giving prednisone without antivirals can cause immunosuppression and the patient can end up in the hospital with a severe case of zoster or herpes meningitis. Even though the hallmark sign of vesicles on an erythematous base is not noted, this is a new rash and missing the early stages of zoster can be disastrous for the geriatric patient. Regardless, if it is bullous pemphigoid, the prednisone will help reduce further outbreaks of bullae. Always check for allergies, all antibiotics given within 90 days, and what medications the patient is on. Call the PCP if the patient is on Coumadin so they can repeat the INR early. Diabetics need to be watched for elevations in glucose.
Unfortunately, these patient care settings have higher rates of MRSA infections. The geriatric patient with open wounds and immunosuppression is susceptible. Typically, Doxycycline will treat the differential of bullous impetigo and/or prevent a secondary infection of MRSA, but I like to wait for the culture results to come back before prescribing any antibiotics. There is so much resistance in these facilities, caution should be used prior to prescribing without culture results. I ordered Gentamicin ointment which will help with wound healing and treat any superficial staph or MRSA.
At the next visit, consent from his power of attorney was given for two 4 mm punch biopsies would be performed, one for H&E and one for direct immunofluorenscense (DIF). Make sure the edge of the bulla for the H&E and 2cm from the most current bulla is selected (yes, in an area where no bulla is present!) for the DIF. Make sure the specimen for DIF is placed in Michels solution. The other specimen for H&E in a formalin container. Don’t forget to give the pathologist a description and history to help with the diagnosis.
Are you comfortable with working up this patient? Great! If not, make sure you are signed up for lecture series “It’s Fundamental My Dear Watson: A Sherlockian Approach to Dermatology. Stayed tuned for Part II where workup results are discussed.
See Debra Shelby, PhD, DNP, DCNP, FNP-BC, FACDNP, FAANP speak at a 2018 Skin, Bones, Hearts & Private Parts conference in Myrtle Beach, Pensacola Beach, San Antonio, Las Vegas.