
When should we worry about a young patient who has a cough? Consider this case that could happen any primary care office or urgent care.
A 36 year old female presents with dry cough for 3 days.
She had some fatigue and was having a tough time chasing the toddlers around at the school where she worked.
She had no past medical history and did not have any fever. She did not smoke.
On exam, her lung sounds were diminished the base on the left, she was overweight and had no s3 or s4. She had 1 + bilateral lower extremity edema.
At this point, what are your differentials? COVID? PE? Pneumonia? CHF? Bronchitis?
Because of her cough, a chest ray was performed. It was read by the provider as “concern for infiltrate” and she was referred to the emergency department.
On arrival, as she was tachycardiac with a priority chief complaint, an ekg was performed.
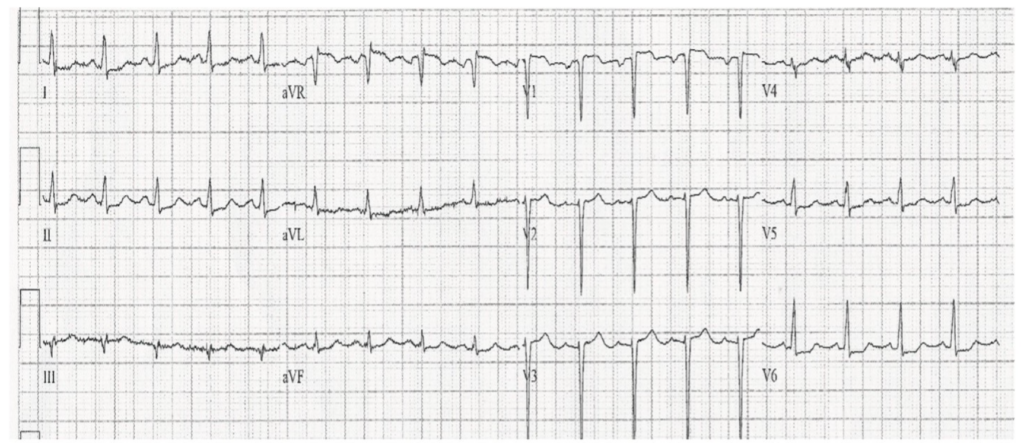
The machine read this as “nonspecific ST T wave changes”.
She also had mild resting tachycardia (HR 109) with no volume loss, normal oxygen saturation. This put PE higher on the diffential and so at the ER aCTA was performed, and no PE was seen.
She did have some minor ST depression in multiple leads and more than 1 mm of ST elevation in AVR. Her Xray was repeated in the emergency department and was read by radiologist as pleural effusion, unilateral and no infiltrate.
Labs were normal except for a BNP of 6929 and a glucose of 310.
Her troponin, cbc and cmp were otherwise normal.
She was subsequently admitted and had a nuclear stress test and was noted to have al low EF of 32% and 95% occlusion of her RCA and 90% in her LAD. The patient ended up getting a CABG.
So how does a 36 y/o F come to Urgent care asking for a Zpak and go home with a CABG?
She was unfortunately diabetic and did not know it and she also had familial hyperlipidemia that was also undiagnosed. These two risk factors meant her “heart age” was a lot older than her chronological age. These two things should make us worry way more about her than the average 36 year old.
This finding warrants immediate angiography according to the new ACC Update Expert Consensus Decision Pathway on the Evaluation and Disposition of Acute Chest Pain in the Emergency Department released in JACC November 15th, 2022. Widespread ST depression with 1 mm of ST elevation as worrisome for involvement of left main and should not wait to be referred to cardiology and should instead go to the ER.
Skin Bones CME In-person Conferences
Hit the reset button while earning continuing medical education credits at our CME conferences, where you can travel to a vacation destination; earn CME credits with like-minded nurse practitioners, physician assistants, and physicians; and ‘unplug’ while enjoying a new locale! Check out our upcoming Skin, Bones, Hearts & Private Parts 2023 CME Conferences and 2024 CME Conferences! At every event, the best of the medical community gathers to earn CME credits, network, and gain knowledge on dermatology, orthopedics, cardiology and emergency medicine, women’s health, pain management and pharmacology, diabetes, ER, and mental health. On-line CME courses and Virtual CME are also available so you have the option of earning CME credits online.