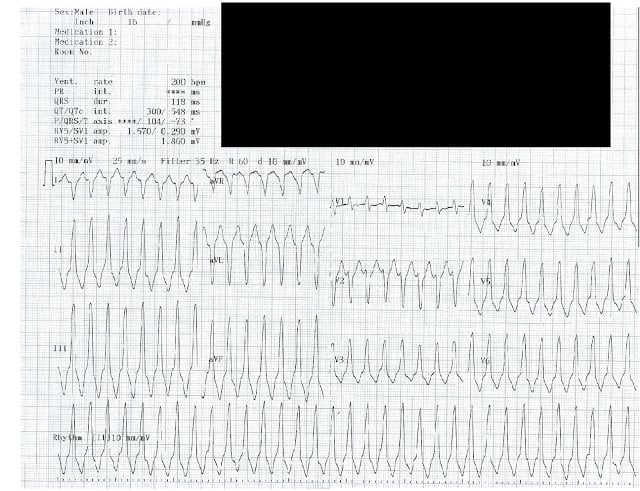
This was a 36 year old female who went to the local urgent care when she got off a plane from a long business trip. She told them she had a cough, and then she also thought she had a “stomach bug” so she took some Imodium. She thought she was going to “walk out of there with an antibiotic” and instead she was taken to the local ER by ambulance. Surprise! Due to her age, she was given adenosine as they thought this was SVT with abberancy. When it didn’t work they did it again. It still didn’t work, so they gave her procainamide, which did work. They was transferred by air to a higher level of care when the flight RN noticed her QTc was long. She was ultimately discharged after she converted, to follow up with cardiology. The thought at the time was that maybe she took too much Imodium (a QT prolonger) or maybe the procainamide did it (also QT prolonging), and that could have caused the VT. (Long qt=Vt or torsades). She went hiking, came back again, and said I don’t feel very good. Her HR was 140 again in a wide complex tachycardia. The ER doctor tried to give her adenosine again, not knowing her history, and she screamed “No, not the stuff with the A”. She was given lidocaine and converted. She ultimately had a VT ablation and is doing well. This is a classic case of VT that doesn’t follow the rules. She is young. Young people are not supposed to have VT. But they can and do. It is less likely but it can happen. This is actually Right Outflow Tract Ventricular Tachycardia and this does not follow the axis rules we have talked about previously. (RVOT) tachycardia is a form of monomorphic VT originating from the outflow tract of the right ventricle or occasionally from the tricuspid annulus. This only accounts for about 10% of all ventricular tachycardias and may respond to adenosine, although hers did not. You always have to rule out Right Ventricular Dysplasia on cardiac MRI, and she did not have it.
See Jennifer Carlquist, PA-C speak in Orlando (April), Myrtle Beach, San Antonio, and Las Vegas.